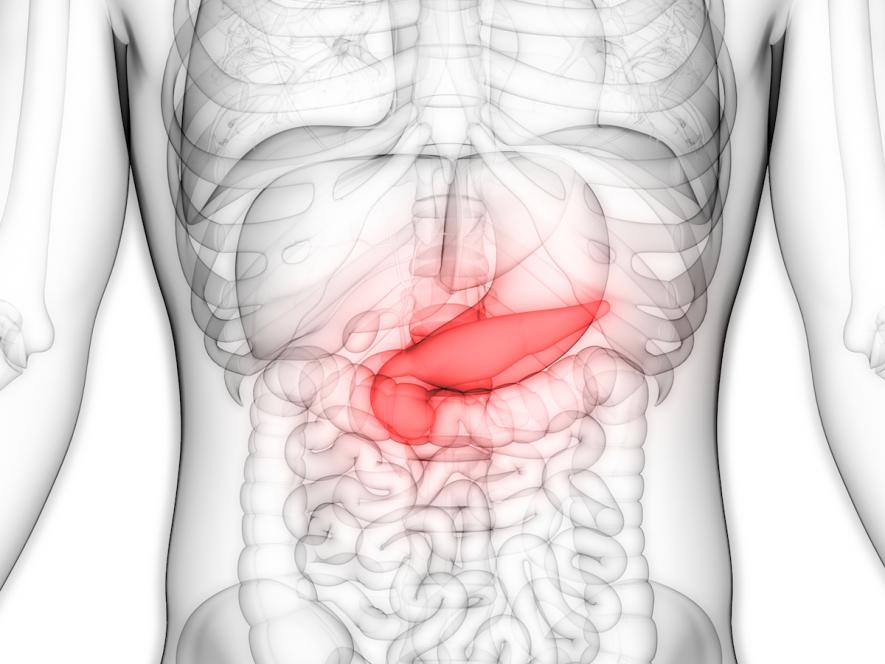
The pancreas is around 22cm long and sits behind the upper section of the abdomen. It is somewhat 'lumpy' in appearance and is larger at one end than the other. The large end is referred to as the 'head', the middle the 'body' and the narrower end is referred to as the 'tail'.
Although known since the time of the ancient Greeks ('pancreas' means 'sweetbread' in Greek), it is only since the late 1800's that medical science has better understood its function in the body.
It has two jobs – the first is to produce enzymes that aid in the digestion of carbohydrates, fats (lipids) and proteins in ingested food, and the second is to produce a range of hormones to regulate glucose in the blood, including insulin. The first of these functions – helping with digestion – is referred to as the 'exocrine process', and the second – glucose regulation – is referred to as the 'endocrine process'.
There are four conditions that can affect the pancreas – these are…
- Diabetes
- Pancreatitis
- Cystic Fibrosis
- Cancer
Diabetes
Diabetes is where there is a problem in insulin production in the pancreas. With Type 1 diabetes the pancreas has stopped producing any insulin at all, due to an immune reaction which destroys the insulin producing cells. With Type 2 diabetes, insulin resistance results in blood glucose levels rising to a point where the pancreas is simply not able to produce the required amount.
Pancreatitis
This is where the pancreas becomes inflamed. The primary cause of this is long term excess alcohol consumption, but it can also be caused by gallstones becoming stuck in the common bile duct (the pancreatic duct shares the same connection to the duodenum as the gallbladder). Other potential causes of the condition include some types of medication, injury to the pancreas and pancreatic cancer (see below). Read more about pancreatitis here.
Cystic Fibrosis
This inherited disease interrupts the exocrine process and people with the condition produce an excess of mucus which affects the lungs and the gastrointestinal tract. Although there is no cure, it can be managed with enzyme replacement and nutritional supplements.
Pancreatic Cancer
This type of cancer is the 11th most commonly diagnosed cancer in Australia. It predominantly affects people over 65 and men more than women. People with a family history of the condition are at higher risk, as are people with diabetes, smokers and alcoholics. Pancreatic cancer can cause pancreatitis, and conversely, chronic pancreatitis may be implicated in the development of pancreatic cancer.
Can you reduce your risk of problems with the pancreas?
The short answer is 'yes', and this is by avoiding or reducing the risk factors listed above. Clearly cystic fibrosis and Type 1 diabetes cannot be 'avoided' but they certainly can be managed. The main guidelines to lowering your risk profile are those shared with many conditions affecting the gastrointestinal tract, which are…
- Maintain a health weight (primarily via good food choices and physical activity)
- Limiting alcohol consumption
- Not smoking